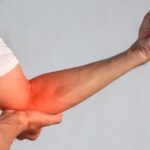
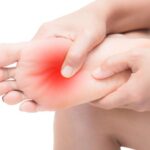
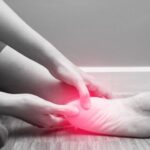
Chronic paresthesia is a disorder that most frequently affects the hands, arms, legs, and feet but can induce numbness or a burning sensation anywhere on the body.
When someone sits for too long on their leg or foot, they experience a “pins and needles” sensation. It is usually a brief sensation caused when pressure is applied to the nerve that supplies a limb. The soreness goes away once the pressure is released.
Some patients experience chronic or ongoing paresthesia, which could indicate a more serious nerve issue or injury.
Chronic paresthesia is more common in women than in men.
What is chronic paresthesia?
Chronic paresthesia
Chronic paresthesia is a neurological disorder described by a persistent sensation of tingling, numbness, burning, or prickling in the affected body area.
It could occur as a result of vitamin deficiencies, underlying medical conditions, or nerve damage. Patients with chronic paresthesia might feel less touched or have problems controlling their motions.
It is estimated that up to 40% of people in the United States experience chronic paresthesia at some point in their lives.
What are the symptoms of chronic paresthesia?
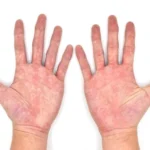
Any area of the body can experience chronic paresthesia, although it most frequently affects the following:
- Hands
- Arms
- Legs
- Feet
The symptoms often include feelings of:
- Numbness
- Weakness
- Tingling
- Burning
- Cold
Having chronic paresthesia might hurt like a stabbing. This could make the affected limb uncomfortable. Walking can be difficult when your legs and feet are affected by paresthesia.
What are the main causes of chronic paresthesia?
Paresthesia that persists could be a symptom of nerve injury. Radiculopathy and neuropathy are two different forms of nerve injury.
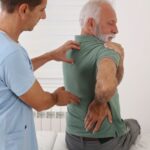
Radiculopathy
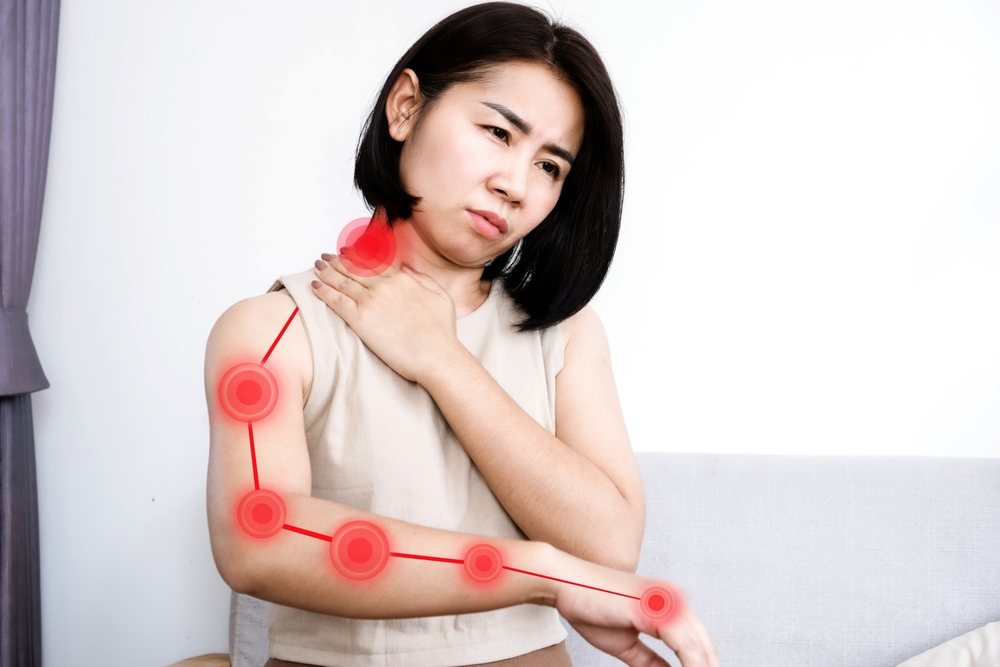
Radiculopathy
The nerve roots’ compression, irritation, or inflammation is a disorder known as radiculopathy. This could happen if you have the following:
- A herniated disc that is putting pressure on a nerve.
- A constriction of the passageway through which the nerve leaves your spinal cord and travels to an extremity.
- Any obstruction in the spinal column that pulls on the nerve as it leaves.
Types of Radiculopathy
There are different types of radiculopathy according to the affected region. These are as follows:
- Cervical radiculopathy
- Lumbar radiculopathy
- Sciatic nerve compression
Cervical radiculopathy
The nerves that give your arms sensation and strength are affected by cervical radiculopathy. The following symptoms could occur if you have cervical radiculopathy:
- Chronic neck discomfort
- Paresthesia in the upper body
- Weakened arm
- Weakness in the hands
Lumbar radiculopathy
Lumbar radiculopathy refers to radiculopathy that affects your lower back. Your leg or foot may have paresthesia if you have lumbar radiculopathy.
Sciatic nerve compression
Compression of the sciatic nerve can happen in more serious situations, which can cause weakness in your legs.
Neuropathy

Neuropathy
Chronic nerve injury leads to neuropathy. High blood sugar, often known as hyperglycemia, is the most frequent cause of neuropathy.
Many other potential causes of neuropathy are:
- Shocks or trauma
- Recurring movement disorders
- Autoimmune conditions like rheumatoid arthritis
- Neurological conditions like multiple sclerosis
- Nephrotic syndrome
- Liver issues
- Stroke
- Brain tumors or tumors close to nerves
- Abnormalities of the bone marrow or connective tissue
- Hypothyroidism
- Vitamin B-1, B-6, B-12, E, or niacin deficits
- Certain pharmaceuticals, including chemotherapy drugs
- Overdosing on vitamin D
- Exposure to harmful elements like toxins or heavy metals
Damage to the nerves can eventually result in paralysis or permanent numbness.
How is paresthesia diagnosed?
Your doctor will likely conduct a complete physical examination. This will likely include a neurological evaluation as well.
- Blood tests and other laboratory techniques, such as spinal taps, may be able to rule out some illnesses.
- If your doctor thinks you have a neck or spinal condition, they can recommend imaging tests like X-rays, CT scans, or MRI scans.
- Depending on the results, they might suggest a neurologist, orthopedist, endocrinologist, or another specialist.
What are the treatments for chronic paresthesia?
Several medications may be useful if you have chronic paresthesia that does not go away despite treating an underlying issue. It includes:
- Painkillers available over the counter, such as acetaminophen and ibuprofen.
- Topical remedies like lotions with anti-inflammatory ingredients and capsaicin.
- Oral prescription medicines such as pregabalin and gabapentin.
Physical therapy
Exercise and physical therapy effectively build muscles and ease the signs and symptoms of bone and muscle injuries.
Surgery
When non-operative methods of treating chronic paresthesia are unsuccessful, in that case, you might be a candidate for surgery, such as a carpal tunnel release or spinal fusion, to cure chronic numbness caused by nerve retention or compression.
What is the prognosis for those who have paresthesia?
You might have chronic paresthesia if those abnormal sensations don’t disappear or return too regularly. In addition, the severity of the symptoms may make routine chores more challenging.
- It is essential to identify the cause of the issue for this reason. Never hesitate to seek a second view or advice from a professional if necessary.
- How severe and how long-lasting persistent paresthesia will depend on the underlying cause. Sometimes, addressing the underlying problem resolves the issue.
- If your present course of treatment isn’t working, let your doctor know so that a different line of action can be taken.
Can chronic paresthesia be prevented?
Sometimes it’s impossible to prevent paresthesia. For instance, if you frequently nod off while holding your arms, you probably can’t help it.
However, you can take steps to reduce the frequency or severity of paresthesia. As an illustration, wearing wrist splints at night may lessen compression on your hand’s nerves and help with paresthesia symptoms.
Follow these steps to avoid chronic paresthesia:
- Aim to limit your exposure to repetitive motion.
- If you perform repetitive motions, stop frequently.
- Get up and move around as often as possible if you sit still for an extended period.
- If you have diabetes or any chronic condition, careful observation and management of illness will reduce your risk of chronic paresthesia.
When should someone with chronic paresthesia visit a doctor?
Consult your physician if:
- Your symptoms may fluctuate or progressively get worse.
- The symptoms appear to be connected to specific activities.
- You feel lightheaded or have muscle cramps.
- You’ve got a rash.
- As you move, your leg symptoms get worse.
- Both sides of your body are affected by your symptoms.
- Your arm or leg, namely one of your fingers or toes, feels numb.
Related Posts:
How To Relieve The Pain of Pinched Nerve